Sleep Apnea
Understanding Sleep Apnea
Sleep apnea is a common term for breathing disruptions and respiratory disorders experienced during sleep that can have serious health consequences if left untreated.
The most common form, known as obstructive sleep apnea (OSA), affects at least 9% of the adult population and is significantly underdiagnosed. During sleep, most muscles in our bodies relax completely, but muscles of the upper airways normally maintain some tone to keep the airways open and allow proper breathing. For people with sleep apnea, however, this critical airway support fails.
How Obstructive Sleep Apnea Occurs
Their airway muscles relax excessively, causing airway collapse and one of two types of breathing events:
Health Impact and Severity Measurement
Both types of breathing events lead to dangerous reductions in blood oxygen levels, which cause immediate detrimental effects on normal brain function and cardiovascular health. The apnea-hypopnea index (AHI)—the mean number of apnea and hypopnea events per hour of sleep—is used to assess the severity of obstructive sleep apnea and determine appropriate treatment options such as CPAP therapy.
What is Sleep Apnea?

Sleep Apnea
Sleep Apnea
Sleep apnea is a serious sleep disorder characterized by repetitive breathing pauses during sleep lasting 10 seconds to several minutes. These interruptions can occur hundreds of times per night, causing poor sleep quality, drops in blood oxygen levels, and serious health consequences including cardiovascular disease, stroke, and diabetes.
Types of Sleep Apnea:
– Obstructive Sleep Apnea (OSA) – Most common; caused by airway collapse
– Central Sleep Apnea (CSA) – Brain fails to signal breathing muscles
– Complex Sleep Apnea – Combination of OSA and CSA
Sleep Apnea Severity (AHI Score):
Mild: 5-15 events/hour
Moderate: 15-30 events/hour
Severe: 30+ events/hour
Obstructive Sleep Apnea (OSA) occurs when throat muscles relax excessively during sleep, causing partial or complete airway blockage. Symptoms include loud snoring, gasping, choking, and breathing pauses often noticed by bed partners.
Early sleep apnea diagnosis and CPAP therapy can dramatically improve sleep quality and reduce health risks.
Sleep Apnea Signs and Symptoms
What are the signs and symptoms of sleep apnea?
Nighttime Symptoms:
– Loud, chronic snoring
– Breathing pauses during sleep (often noticed by bed partners)
– Gasping or choking during sleep (may wake you suddenly)
– Fragmented or restless sleep
– Dry mouth or sore throat upon awakening
Daytime Symptoms:
– Excessive daytime sleepiness and chronic fatigue
– Not feeling refreshed in the morning
– Morning headaches due to oxygen deprivation
– Difficulty concentrating and memory problems
Health Warning Signs:
– High blood pressure (hypertension)
– Increased cardiovascular risk
– If you experience multiple symptoms, consult a sleep medicine professional for a sleep apnea test. Early CPAP therapy can improve sleep quality and health outcomes.
Other Sleep Apnea Common Signs and Symptoms
What are other common sleep apnea signs and symptoms?
Cognitive & Emotional:
– Mood swings, irritability, and depression
– Poor concentration, decreased attention, and memory loss
– Lack of energy and decreased work performance
Physical & Risk Factors:
– Sexual dysfunction and decreased libido
– Large neck circumference (over 17″ men, 16″ women)
– Being overweight or obese
– Frequent nighttime urination (nocturia)
Serious Health Indicators:
– Impaired alertness while driving (drowsy driving risk)
– History of heart attack or stroke
– Increased cardiovascular disease risk
– If you have multiple symptoms, schedule a sleep apnea test. CPAP therapy can improve energy, cognitive function, and reduce cardiovascular risks.
Health Risks of Untreated Sleep Apnea
What are the health risks of untreated sleep apnea?
Untreated obstructive sleep apnea can lead to serious, life-threatening complications:
Cardiovascular Risks:
– Heart disease, heart attack, and stroke
– High blood pressure (hypertension)
– Irregular heartbeat (arrhythmia)
Metabolic & Other Health Risks:
– Type 2 diabetes and insulin resistance
– Sexual dysfunction and impotence
Safety Risks:
– Fatigue-related motor vehicle accidents
– Workplace accidents due to excessive daytime sleepiness
Severe Consequences:
– Premature death and reduced life expectancy
Early diagnosis and CPAP therapy can significantly reduce these health risks and improve quality of life.
Who is at Risk
Who is at risk for sleep apnea?
Obstructive sleep apnea occurs in both sexes and all age groups, including children, but is more common in men.
Sleep Apnea Statistics:
– 1 in 5 adults has at least mild sleep apnea
– 42 million Americans have sleep apnea
– 80% are unaware and remain undiagnosed
– 25% of men and 9% of middle-aged women have sleep apnea
Sleep Apnea Risk Factors:
– Male or post-menopausal female
– Being overweight or obese
– Large neck circumference (over 17″ men, 16″ women)
– Large tonsils, tongue, or uvula
– History of high blood pressure, diabetes, stroke, or heart attack
– Excessive use of alcohol, sedatives, and antihistamines
– Family history of sleep apnea
Take Action: If you have sleep apnea symptoms or risk factors, consult a sleep medicine professional immediately. CPAP Expert Clinic can help arrange a home sleep apnea test or sleep study. Contact us at 905-787-7272.
Diagnostic methods

How is Sleep Apnea Diagnosed?
How is sleep apnea diagnosed?
Sleep apnea diagnosis starts with completing a sleep apnea screening test that includes clinically recognized surveys:
– Sleep Apnea Symptom Assessment
– Epworth Sleepiness Scale (ESS) – Measures excessive daytime sleepiness
– Berlin Questionnaire – Evaluates sleep apnea risk factors
Next Steps: If you scored positive or suspect sleep apnea symptoms, consult a sleep medicine professional to discuss further diagnostic testing.
Diagnostic Testing Options:
– In-Lab Sleep Study (Polysomnography/PSG) – Comprehensive overnight sleep study conducted in an accredited sleep laboratory
– Home Sleep Apnea Test – Convenient, portable monitoring device for at-home sleep apnea screening and preliminary diagnosis
CPAP Expert Clinic can help arrange your sleep apnea test. Contact us at 905-787-7272 for assistance.
Full Sleep Study (PSG)
What is Polysomnography (PSG)?
Polysomnography (PSG) is a comprehensive overnight sleep study covered through OHIP that records bio-physiological changes during sleep.
PSG is the gold standard diagnostic test used to assess sleep quality, diagnose obstructive sleep apnea, and rule out other sleep disorders that negatively affect health.
What Does a PSG Test Monitor?
– A PSG test objectively measures:
– Brain wave activity (EEG)
– Eye movements (EOG)
– Muscle activity in legs and chin (EMG)
– Heart rate and rhythm (ECG)
– Respiratory effort and nasal airflow
– Blood oxygen levels (SpO2)
– Body position
– Snoring patterns
What to Expect During the Sleep Study:
– Non-invasive setup: Monitoring sensors and electrodes are safely attached using gentle adhesive or gel paste (easily removed with soap and water)
– Setup time: Approximately 30 minutes
– Sleep time: Patients go to bed around 10-11 PM and are released by 6-7 AM
– Total visit: Similar to spending a night in a hotel, approximately 10 hours
– Comfort: Painless, non-invasive process
After Your Sleep Study:
Your sleep study results will be thoroughly analyzed by a sleep medicine physician who will provide specific treatment recommendations, including CPAP therapy options if obstructive sleep apnea is diagnosed. A copy of your comprehensive sleep report will be sent to your primary care physician.
In-Home Sleep Apnea Screening Study
What is an In-Home Sleep Apnea Test?
An in-home sleep apnea test may be considered if:
– You want immediate sleep apnea screening in the comfort of your own home
– Your physician wants to pre-screen for obstructive sleep apnea and determine urgency for a full sleep study (PSG)
– You prefer convenient at-home testing with a simple, easy-to-use portable monitoring device
What Does Home Sleep Testing Monitor?
The portable sleep apnea test device measures:
– Respiratory effort and nasal airflow (breathing patterns)
– Heart rate and blood oxygen saturation levels (SpO2)
– Sleep position and movement
The FDA-approved device is provided by our certified Respiratory Therapist and is widely used for sleep apnea screening.
Important Limitations:
An in-home sleep apnea test has limitations and is not a substitute for comprehensive polysomnography (PSG) performed at an accredited sleep laboratory. It provides a preliminary sleep apnea diagnosis to help your sleep medicine physician determine if you need an immediate full sleep study.
Next Steps:
Based on your home sleep test results, your physician will recommend appropriate treatment options, including CPAP therapy if obstructive sleep apnea is diagnosed.
Treatment options
Continuous positive airway pressure (CPAP) is the gold standard and most effective treatment for obstructive sleep apnea. CPAP therapy uses a compact CPAP machine that delivers a steady stream of therapeutic air pressure through tubing into a CPAP mask worn during sleep, keeping airways open and preventing breathing disruptions.
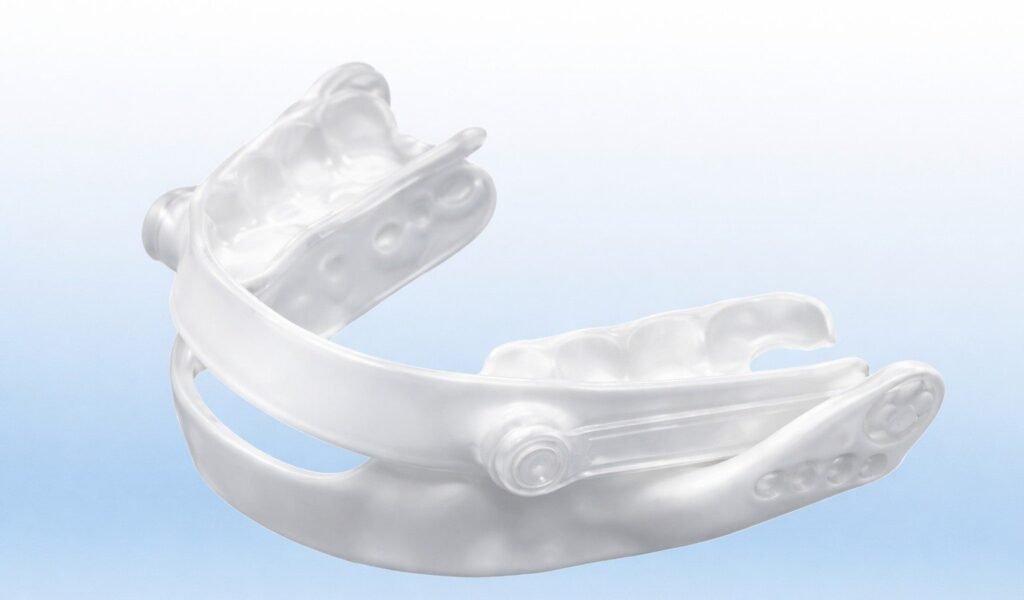
What are oral sleep devices?
Oral appliances (dental sleep devices) are custom-fitted devices designed by dentists specializing in sleep apnea treatment. These mandibular advancement devices keep the lower jaw positioned forward during sleep to prevent airway collapse and may be an alternative treatment option for patients with mild obstructive sleep apnea or those unable to tolerate CPAP therapy.

Weight loss help sleep apnea?
Sleep apnea severity is strongly associated with excess weight and obesity. Weight loss can dramatically improve obstructive sleep apnea symptoms, reduce apnea-hypopnea index (AHI) scores, and may decrease CPAP pressure requirements. Combined with CPAP therapy, achieving a healthy weight provides significant health benefits and better treatment outcomes.
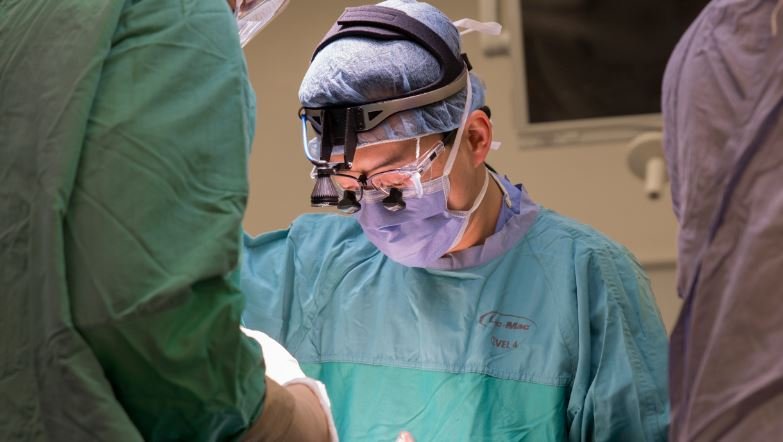
Is surgery an option for sleep apnea?
Surgical intervention may help some obstructive sleep apnea patients, particularly those with enlarged tonsils, adenoids, nasal polyps, deviated nasal septum, or jaw abnormalities. Surgery can enlarge airways or tighten airway muscles to reduce sleep apnea severity. However, for most patients, surgical results are temporary as sleep apnea symptoms often return over time. CPAP therapy remains the most effective long-term treatment for sustained symptom relief and health outcomes.

What lifestyle changes help with sleep apnea?
Avoiding alcohol before bedtime reduces obstructive sleep apnea severity by preventing excess throat muscle relaxation. Sleeping pills and muscle relaxants should also be avoided as they exacerbate sleep apnea symptoms and airway collapse. Consult your sleep medicine physician to determine if your medications are worsening symptoms and to optimize CPAP therapy effectiveness.
Benefits of successful treatment

Reduce the risk of stroke, heart and blood pressure problems

Decrease blood glucose levels by decreasing insulin resistance

Reduce feelings of daytime fatigue and sleepiness
Decrease oxidative stress and inflammation in the body

Improve the patients and their bed partners quality of life
Better Sleep Equals Better Life
Better sleep equals better life—poor sleep negatively impacts cardiometabolic health, cognitive function, and overall quality of life. CPAP therapy and assistive sleep devices help treat obstructive sleep apnea, improve sleep quality, and allow your body to naturally heal and restore during restorative sleep. If you’re struggling with untreated sleep apnea or experiencing CPAP therapy challenges, CPAP Expert Clinic is here to help!

