Resources
Most Common Sleep Disorders
Sleep disorders are conditions that prevent restful sleep and restorative rest, resulting in excessive daytime sleepiness, chronic fatigue, and impaired daily functioning. There are approximately eighty different types of sleep disorders affecting millions of people. The most common sleep disorders include obstructive sleep apnea, insomnia, restless leg syndrome, narcolepsy, and circadian rhythm disorders. Early diagnosis and appropriate treatment can dramatically improve sleep quality, daytime energy, and overall health outcomes.
Snoring
Snoring is a common sleep-related breathing disorder affecting millions of adults. The noise occurs when inhaled air vibrates over relaxed throat tissues and soft palate during sleep, causing airway turbulence.
Understanding Snoring
While snoring can be simply a noise issue that disturbs bed partners, it may also be a warning sign of obstructive sleep apnea—a serious sleep disorder requiring medical attention. Snoring occurs more frequently in men, people who are overweight, and tends to worsen with age due to increased throat muscle relaxation.
When Snoring Becomes a Problem
Occasional snoring is usually not serious and is mostly a nuisance for your bed partner. However, habitual snoring (chronic snoring every night) disrupts sleep quality for both you and those close to you, leading to sleep fragmentation, excessive daytime sleepiness, and reduced health outcomes.
Treatment Options
Medical evaluation by a sleep medicine professional is recommended for habitual snorers to rule out obstructive sleep apnea and determine appropriate treatment. Solutions may include lifestyle changes, CPAP therapy for sleep apnea, oral appliances, or positional therapy to improve sleep quality and nighttime breathing.
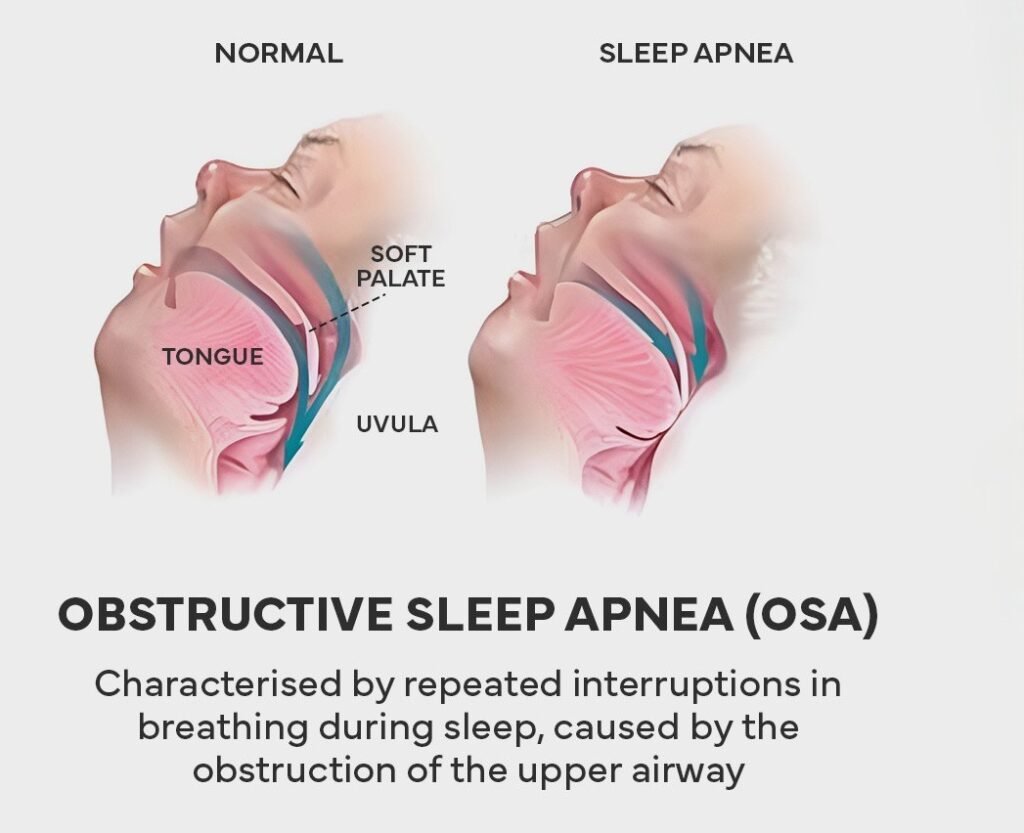
Obstructive Sleep Apnea
Obstructive sleep apnea is a serious sleep disorder that occurs when breathing is repeatedly interrupted during sleep. People with untreated sleep apnea stop breathing hundreds of times during the night due to airway collapse when throat muscles and soft tissues relax excessively.
Understanding Sleep Apnea
There are two types: obstructive sleep apnea (OSA) and central sleep apnea. Obstructive sleep apnea is the most common form, caused by complete or partial airway blockage during sleep. Men, people who are overweight, and individuals over 40 are at greater risk for developing sleep apnea
.
Health Risks of Untreated Sleep Apnea
If left untreated, obstructive sleep apnea can result in serious health problems including high blood pressure, stroke, heart failure, irregular heartbeat, heart attacks, type 2 diabetes, depression, and worsening of ADHD. Untreated sleep apnea also causes excessive daytime sleepiness, leading to poor work and school performance, motor vehicle crashes, and academic underachievement in children and adolescents.
Treatment Options
Sleep apnea testing and CPAP therapy can eliminate breathing disruptions, improve sleep quality, and reduce cardiovascular risks. Consult a sleep medicine professional if you experience chronic snoring, breathing pauses, or daytime fatigue.
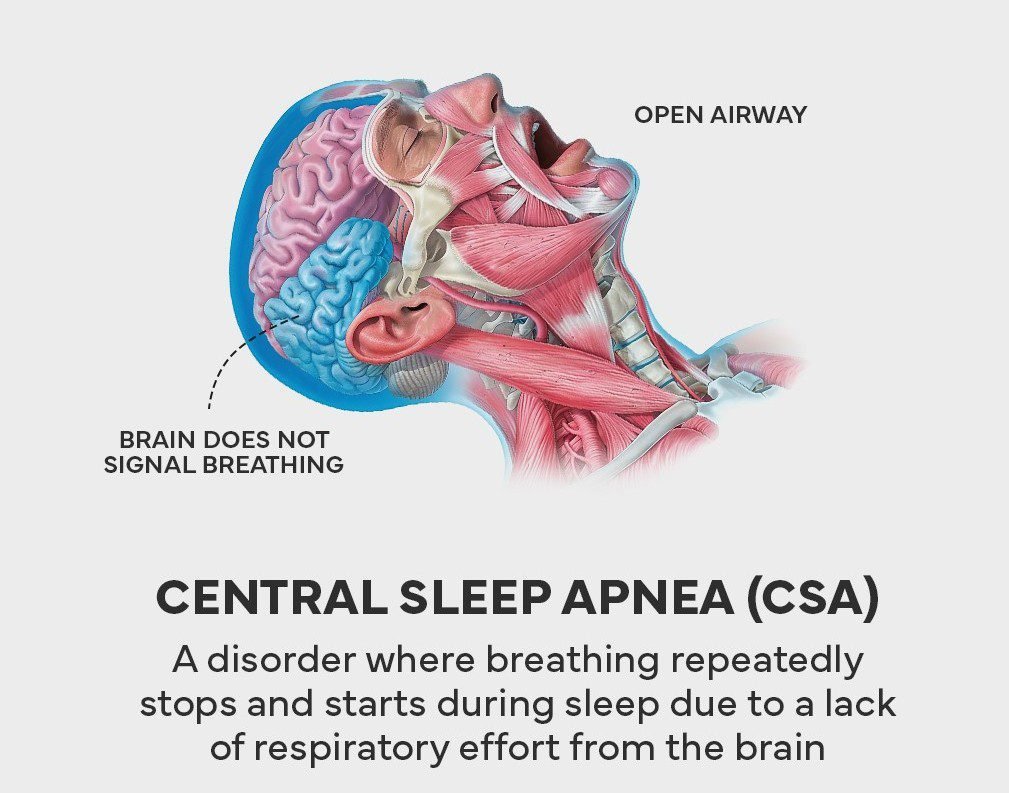
Central Sleep Apnea
In central sleep apnea, breathing is disrupted regularly during sleep due to neurological dysfunction rather than physical airway obstruction. Unlike obstructive sleep apnea where the airway is blocked, central sleep apnea occurs when the brain fails to send proper signals to breathing muscles, causing respiratory pauses during sleep.
Understanding Central Sleep Apnea
Central sleep apnea is related to central nervous system dysfunction and is usually associated with serious underlying medical conditions, particularly those affecting the lower brainstem that controls breathing patterns. This type of sleep apnea requires specialized medical evaluation and treatment by sleep medicine professionals.
Conditions Associated with Central Sleep Apnea
Treatment for central sleep apnea focuses on managing underlying medical conditions and may include specialized PAP therapy devices such as BiPAP or adaptive servo-ventilation (ASV). Consult a sleep medicine professional for proper diagnosis and comprehensive treatment planning.
Insomnia
Insomnia is a common sleep disorder where people struggle to get adequate restful sleep at night. Individuals with insomnia may have difficulty falling asleep, experience frequent nighttime awakenings, or wake up too early in the morning, leading to poor sleep quality and excessive daytime sleepiness.
Common Causes of Insomnia
Treatment may include cognitive behavioral therapy for insomnia (CBT-I), improved sleep hygiene, and addressing underlying sleep disorders. Consult a sleep medicine professional for proper diagnosis and treatment to improve sleep quality.
Circadian Rhythm Disorder
Circadian rhythm disorders are disruptions in a person’s internal body clock—the biological system that regulates the 24-hour sleep-wake cycle. These sleep disorders occur when your natural circadian rhythm is misaligned with your environment or schedule, causing sleep pattern disruptions.
Symptoms and Impact
Individuals with circadian rhythm disorders experience insomnia at certain times and excessive daytime sleepiness at others, resulting in impaired work performance, school difficulties, and reduced quality of life.
Common Types
– Jet lag – Sleep disruption from crossing time zones
– Shift work sleep disorder – Sleep problems from night shifts or rotating schedules
– Delayed sleep phase syndrome – Falling asleep and waking too late
– Advanced sleep phase syndrome – Falling asleep and waking too early
Treatment Options
Treatment may include light therapy, melatonin, sleep schedule adjustments, and improved sleep hygiene. Consult a sleep medicine professional for proper diagnosis and treatment.
Jet Lag
Jet lag, also known as time-zone change syndrome, is a temporary circadian rhythm disorder and sleep pattern disruption following travel across multiple time zones. This common sleep disorder occurs when your internal body clock cannot immediately adjust to the new time zone.
Symptoms of Jet Lag
As the body struggles to cope with the new sleep-wake schedule, travelers may experience:
Who Is Affected?
Jet lag is a common problem for travelers, particularly those over 50 compared to those under 30. Severity varies depending on the number of time zones crossed and direction of travel (eastward travel typically causes worse jet lag). Symptoms may appear one to two days after travel, and frequent travelers can develop chronic jet lag symptoms affecting quality of life.
Shift Work Sleep Disorder (SWSD)
Shift work sleep disorder (SWSD) is a circadian rhythm disorder that affects people who frequently rotate shifts or work night shifts, disrupting their natural sleep-wake cycle.
Work schedules of these individuals go against the body’s natural circadian rhythm and internal body clock, making it difficult to adjust to different sleep and wake schedules. SWSD consists of a constant or recurrent pattern of sleep disruption that results in insomnia or excessive daytime sleepiness. This sleep disorder is common in people who work non-traditional hours, usually between 10:00 p.m. and 6:00 a.m.
Common Symptoms of SWSD
Managing Shift Work Sleep Disorder
Shift workers must prioritize sleep quality and sleep hygiene. People who work shifts other than a 9:00 a.m. to 5:00 p.m. routine might have to prepare for sleep during daylight hours. Prepare your body and mind for restful sleep. Minimize light exposure on your way home from night shifts to prevent morning sunlight from activating your internal body clock. Follow consistent bedtime rituals and try to keep a regular sleep schedule—even on weekends. Go to sleep as soon as possible after work. It is essential to get at least 7 to 8 hours of quality sleep every day to maintain health outcomes and therapy adherence.
Periodic Limb Movements Disorder (PLMD)
Periodic Limb Movement Disorder (PLMD) is a sleep disorder characterized by repetitive cramping or involuntary jerking of the limbs during sleep. The movements typically involve the legs, but upper extremity movements may also occur, disrupting sleep quality and causing sleep fragmentation.
“Periodic” refers to the fact that the movements are repetitive and rhythmic, occurring about every 20-40 seconds. They tend to cluster in episodes that last anywhere from a few minutes to several hours. PLMD is considered a sleep disorder because the movements often disrupt restful sleep and lead to excessive daytime sleepiness and chronic fatigue.
Causes of PLMD
The causes of PLMD are unknown. However, recent research has shown that people with a variety of medical conditions, including Parkinson’s disease, narcolepsy, and other neurological disorders, may have frequent periodic limb movements during sleep. PLMD may also be caused by certain medications, most notably antidepressants and other psychotropic drugs.
Symptoms of PLMD
The most common symptoms reported by people with PLMD are poor sleep quality, sleep disruption, and excessive daytime sleepiness. Many people with PLMD are unaware of their leg movements unless their bed partner or sleep study reveals them.
Characteristics of Limb Movements:
Restless Legs Syndrome (RLS)
Restless Legs Syndrome (RLS) is a neurological sleep disorder that causes uncomfortable tingling, pulling, creeping, or painful sensations in the legs, disrupting sleep quality and causing sleep fragmentation.
Understanding RLS
In people who have Restless Legs Syndrome, discomfort in the legs and feet peaks during the evening and nighttime hours. They feel an uncontrollable urge to move their legs and feet to get temporary relief, often resulting in excessive, rhythmic, or cyclic leg movements during sleep similar to periodic limb movements. This sleep disruption can delay sleep onset and significantly disrupt restful sleep, leading to excessive daytime sleepiness, chronic fatigue, and reduced quality of life.
Managing Restless Legs Syndrome
Narcolepsy
Narcolepsy is a chronic neurological sleep disorder that affects the brain’s ability to regulate the sleep-wake cycle, causing excessive daytime sleepiness and sudden sleep attacks. There is sometimes a genetic component, but most patients have no family history of the sleep disorder. It may start in childhood but typically peaks in young adulthood.
Understanding Narcolepsy
Narcolepsy is characterized by extreme, overwhelming daytime sleepiness and loss of alertness during the day. It is caused by a dysfunction of the brain mechanisms controlling sleep and waking, often related to low levels of hypocretin (orexin), a brain chemical that regulates wakefulness. The person may suddenly fall asleep mid-sentence, while at work, or behind the wheel of a car, creating serious safety risks. Other symptoms of narcolepsy include cataplexy (the sudden loss of muscle tone while awake, when surprised or upset, which can be severe enough to cause a collapse), vivid hallucinations as the person is falling asleep, and sleep paralysis.
Diagnosis and Treatment
The symptoms of narcolepsy can be found in several other sleep disorders, including obstructive sleep apnea and other conditions causing excessive sleepiness, so accurate diagnosis through sleep testing is critical. Consult a sleep medicine professional for proper evaluation. Treatment options may include medications to promote wakefulness, improve sleep quality at night, and manage cataplexy symptoms.
Night Terrors and Nightmares
Night Terrors
Night terrors are a sleep disorder that occurs most often in children between the ages of 3 and 5 years old, during deep non-REM sleep stages. A night terror episode can be dramatic: your child may wake up screaming, appearing terrified and disoriented, but unable to explain the fear or be consoled.
Sometimes children who have night terrors remember a frightening image, but often they remember nothing about the episode. Though night terrors can be alarming for parents who witness them, they’re not usually a cause for concern or a sign of a deeper medical issue or underlying sleep disorder. Most children outgrow sleep terrors by adolescence as their sleep patterns mature.
Nightmares
Nightmares are disturbing dreams associated with negative feelings, such as anxiety, fear, or stress. Nightmares seem real, often becoming more disturbing as the dream unfolds during REM sleep. Nightmares can be triggered by a frightening or stressful event, a fever or illness, or the use of some medications, alcohol, or sleep deprivation. They may begin in childhood and tend to decrease after about age 10. However, some people have them as teens or adults, or throughout their lives.
Nightmares may become a problem if you have them frequently and they cause you to fear going to sleep, disrupt sleep quality, or keep you from getting restful sleep. If nightmares persist and affect daytime functioning or sleep quality, consult a sleep medicine professional for evaluation and potential treatment options.
Accredited Sleep Clinics in Ontario
Brampton
Brampton Sleep Clinic
P. 905-456-3699
40 Finchgate Boulevard
Suite 216
Brampton ON L6T 3J1
Markham
Woodbine Steeles Sleep Clinic
P. 416-628-4010
7155 Woodbine Avenue
Suite B103
Markham ON L3R 1A3
Mississauga
Tri-Hospital Sleep Laboratory West
P. 905-566-1010
3024 Hurontario Street
Suite 208
Mississauga ON L5B 4M4
Etobicoke
Brain and Sleep Diagnostic Centre
P. 416-231-5770
135 Queen’s Plate Drive
Suite 140
Etobicoke ON M9W 6V1
Thornhill
Toronto Sleep Institute
P. 905-709-9696
7099 Yonge Street
Suite 205
Thornhill, ON L3T 0H1
North York
Appleton Clinic
P. 416-635-0909
845 Wilson Ave
Suite 301
North York, ON M3K 1E6
Toronto
Centre for Sleep and Chronobiology Sleep Disorders
P. 416-603-9531
295 College St.
Suite 301
Toronto, ON, M5T 1S2
SLEEP CARE Solutions Yonge & Davisville
P. 416-792-9436
1849 Yonge Street
Suite 303
Toronto ON M4S 1X8
